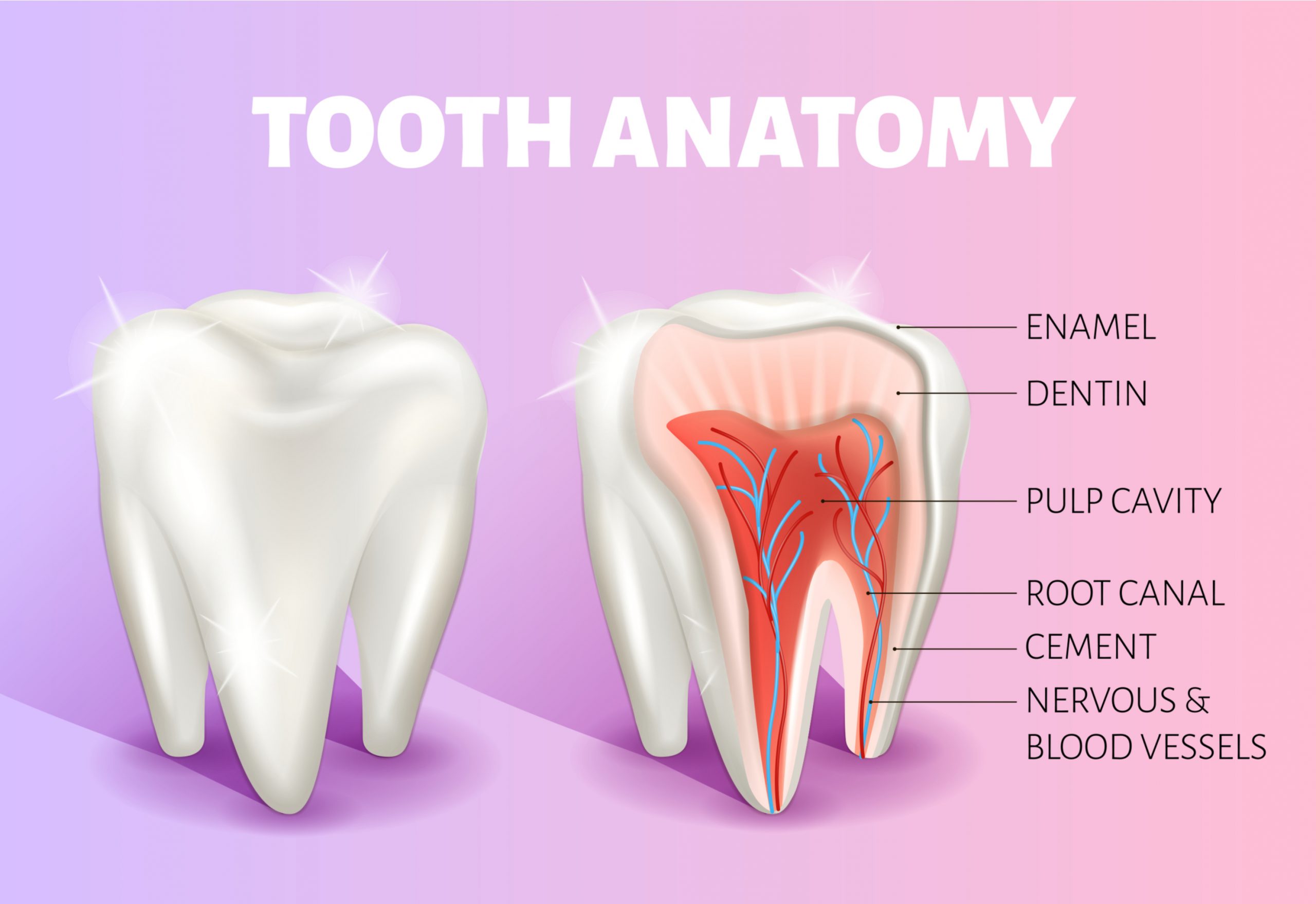
Root Canal Treatment:
Root canal Treatment is a sequence of procedures involving the pulp of the tooth, which results in the elimination of infection and protection against future microbial infection. This treatment involves removal of contents and cleaning of the infected pulp chamber using a series of instruments.
A brief description about the tooth anatomy
Progress of Tooth Decay
- Caries: The main cause of tooth decay is food that gets stuck on the teeth. Foods rich in sugar content are broken down by bacteria present in the mouth into acid that damages the tooth surface and over a period of time causes a hole in the tooth.
- Enamel Caries: This is the tooth decay limited to the outer strong protective covering of the tooth. During this stage the decay may be visible clinically and there are limited symptoms of sensitivity or pain
- Dentin Caries: In this stage the decay has breached the outer protective covering and reached the inner layer of dentin. During this stage there may be sensitivity to hot and cold and occasional pain in the tooth lasting for a few minutes.
- Pulpitis: It is the inflammation of the dental pulp. Decay of the tooth which leads to cavities, eventually extends beyond the enamel, dentin and reaches the pulp. At this point, the pulp reacts to the exposure of bacteria present in the mouth with a reaction, which is called pulpitis. Pulpitis results in a tooth ache which is acute and painful. Pulpitis also presents with increased sensitivity to hot and cold food. It is also seen that pulpitis can sometimes occur without pain. Pulpitis is also caused by the trauma to the tooth, exposure to extreme hot and cold foods, and overheating of the dental instruments (Dental Hand piece) in contact with the tooth during treatment.
Tests are conducted to evaluate the nature of the pulpitis. Tests conducted are mostly thermal with the help of ethyl chloride and electrical using the electric pulp tester.
- Pulpitis can be classified into two types:
- Reversible pulpitis
- Irreversible pulpitis
Reversible Pulpitis:
- It is a mild to moderate condition of the pulp caused by noxious stimuli in which the pulp is capable of returning to the normal, uninflamed state, following the removal of stimuli. Symptomatic reversible pulpitis is characterized by sharp pain lasting for a moment. It is more often brought on by cold, than hot food or by beverages and by cold air.
- Clinically, the difference between reversible & irreversible pulpitis is quantitative, the pain of irreversible pulpitis is more severe & lasts longer. The best treatment for reversible pulpitis is prevention. Periodic care is required to prevent the development of caries, and early insertion of a filling is recommended, if a cavity has developed.
Irreversible Pulpitis
- It is the persistent inflammatory condition of pulp, either symptomatic or asymptomatic, caused by a noxious stimulus. The pain may persist for several minutes to hours, lingering, after removal of a thermal stimulus. Most common cause is bacterial involvement of pulp through caries.
- Any clinical, chemical or thermal factor can also cause irreversible pulpitis. In early stages, a paroxysm of pain is caused by sudden temperature changes, particularly cold. The pain often continues when the cause has been removed. The patient may describe the pain as sharp, piercing or shooting and it is generally severe. It may be intermittent or continuous depending on the degree of involvement of pulp.
- The patient may also have pain referred to adjacent teeth, sinuses or to the temple when upper posterior teeth are involved. In later stages, the pain is more severe and is generally described as boring, gnawing or throbbing.
Internal Resorption
- In cases when the pulpitis is chronic, osteoclastic activity begins in the pulp chamber which causes a fast progressive resorptive process occurring in the dentin of the pulp chamber or root canals of teeth. Internal resorption is usually seen to be associated with trauma to the tooth. In internal resorption, the root of the tooth is asymptomatic.
- In the crown, it is manifested as a reddish area called “pink spot”. The affected tooth is also known as “Pink tooth of mummery”. The reddish area represents the granulation tissue showing through the resorbed area of crown.
- Extirpation of the pulp, stops the internal resorptive process. In many patients, the condition progresses unobserved because it is painless, until the root is perforated. In such a case, mineral trioxide aggregate (MTA) is recommended to repair the defect. When the repair has been completed, the canal with its defect is obturated with plasticized gutta-percha.
When is Root Canal Treatment required?
- Root canal treatment is required when the pulp is inflamed, and the soft tissue inside the pulp chamber is infected.
- Deep decay
- Injury to the tooth
- Irreversible pulpitis
Symptoms of Root canal
- Severe pain in the tooth
- Sensitivity to hot or cold foods
- Pain in the tooth while touching the opposing tooth
- Pain due to fracture or injury to the tooth
- Swollen gums next to the tooth
- Deep decay or damage to the tooth structure
Procedural Steps
A root canal is typically done by an endodontist or a general dentist. The root canal might be done in a single or may require multiple visits. A root canal typically has three steps.
- Opening the tooth (Access opening)
- First, the dental X-ray is taken to note the extent of damage.
- An anaesthesia is administered to manage pain, which can be quite severe if the tooth is septic.
- Then a rubber-like sheet known as a dental dam is place in your mouth to keep the tooth dry, clean, protected and free from saliva. Or the dentist may use sterilized cotton rolls for the same purpose.
- Cleaning and shaping (Debridement)
- Decay is removed from the surface of the tooth, and a small opening is created through the crown of the tooth to gain access to the pulp chamber.
- Using tiny dental instruments, the infected or diseased pulp is removed.
- After the diseased pulp is removed, the pulp chamber and root canals are flushed clean with the help of liquid solutions and mechanical debridement of the inner walls of the root canals.
- The root canals may also be reshaped and enlarged to permit greater access for filling.
- Prior to initiating the filling process, the root canals should be devoid of all infection, and dried. Medication may need to be placed into the pulp chamber, in between appointments, to clear any residual infection. If Infection reaches beyond the tip of the root which is inside the gum, the patient is prescribed antibiotics. If the root canal needs multiple visits, a temporary filling is placed within the crown to guard the tooth from debris and secretions of the oral cavity.
- It is important that the tooth being treated for a root canal be reduced in height to take it out of contact of the opposing tooth (occlusion), thus allowing for healing of the root of the tooth from reduced opposing pressure.
- Filling of the root canal (Obturation)
- After the shaping, cleaning and disinfecting the pulp it is ready for drying of the canals. It is time to fill the inside of the tooth, the empty pulp chamber and root canals. A medicated sealer paste and an inert rubber compound called GuttaPercha is used to fill the tooth, followed by temporary or permanent filling in the crown portion of the tooth.
- Post and Core or Permanent Filling
- As the tooth typically encompasses a large filling or is weakened from extensive decay, it should be shielded from future damage and returned to normal function. Before placing a placing a crown — an artificial tooth resembling a natural tooth, sometimes prior to the placement of a crown, a fibre post is first inserted within the tooth to reinforce strength and provide structural support. If a fibre post is not required, the crown portion of the tooth is covered with dental filling materials (most often composites).
- Crown after Root Canal Treatment
- After your root canal, your tooth needs protection from forces of chewing, which carries the risk of damaging your already weak tooth structure. A crown is placed to provide a strong protective structure to the root canal treated tooth. Different types of crowns are available and the patient can choose as per the requirement and advice of the dentist. The first few days after completion of the root canal, the tooth may be quite sensitive. Pain medications may be prescribed by the dentist to help dealing with pain in these days. If the pain persists visit your dentist for a follow up visit.
We use modern, state-of-the-art technology to treat root canals including the following.
- Digital X-ray equipment
- Digital apex locators
- Rotary filling systems
- Hard and Soft tissue LASERS
- Endodontic Microscopes
- Cone Beam Computed Tomography
Root Canal Treatment is a highly technique sensitive treatment where not only the equipment and materials used, but also the quality of work done by the dentist will determine the prognosis and longevity of the treatment. At Thumbay Dental Hospital, our dentists are experienced professionals who are highly skilled, and shall always provide you with the best quality of dental treatment which is completely pain free.